Surgical treatment for intestinal obstruction in children primarily involves relieving the intestinal blockage through surgical means and restoring normal intestinal function. The goal of the surgery is to directly relieve the obstruction, prevent intestinal necrosis and the spread of infection, and minimize harm to the child.
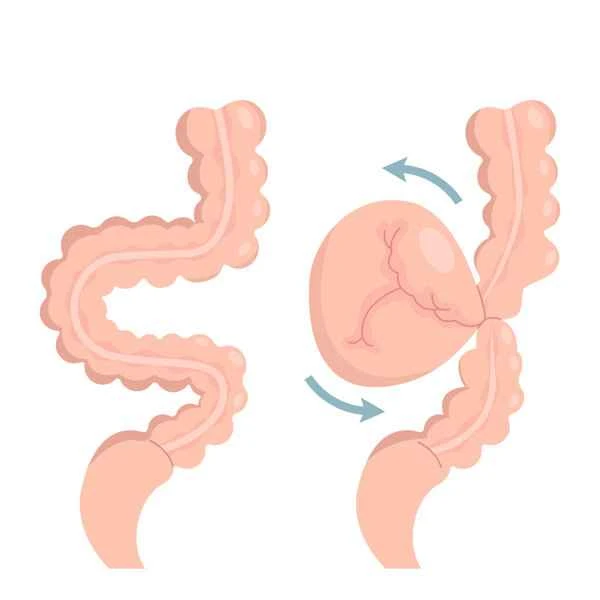
During surgery, doctors will determine the most appropriate surgical approach based on the specific cause, location, severity of the intestinal obstruction, and the child's overall health. If the obstruction is caused by a foreign object or tumor in the intestine, resection may be necessary; if it is caused by intestinal volvulus or adhesions, repositioning or release surgery may be required. During the surgery, doctors will carefully examine every part of the intestine to ensure that no potential obstruction factors are overlooked. Care must also be taken to protect the child's intestinal function and avoid unnecessary damage during the procedure.
Surgical treatment of intestinal obstruction presents doctors with several risks and challenges. The surgery itself may carry risks such as infection and bleeding, while postoperative complications such as intestinal fistula and recurrence of obstruction may arise during recovery. Choosing the appropriate surgical method and postoperative care are crucial for ensuring surgical success. Parents and children need to understand the surgical treatment correctly and avoid excessive anxiety or underestimating the risks. Surgical treatment of intestinal obstruction is a complex process that requires the joint efforts of doctors, parents, and children to ensure the best possible treatment outcome.
[Management Tip:]
1. Closely monitor the child's vital signs and bowel function recovery after surgery.
2. Follow the doctor's instructions and arrange the child's diet and activities reasonably.
3. If abnormal symptoms occur, such as fever or worsening abdominal pain, seek medical attention promptly for a follow-up examination.