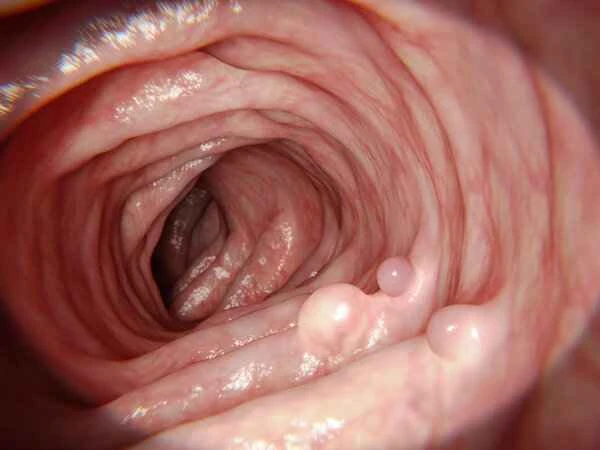
Postoperative intestinal obstruction is a potentially life-threatening complication that occurs after surgery when bowel function is impaired, preventing the normal passage of intestinal contents. The danger of postoperative intestinal obstruction depends primarily on the type, location, duration, and presence of other complications. Intestinal obstruction can hinder normal bowel movements, preventing the expulsion of food residue and gas, leading to symptoms such as abdominal pain, bloating, nausea, and vomiting. If left untreated, intestinal obstruction can cause impaired intestinal blood circulation, resulting in intestinal wall ischemia, necrosis, and even death.
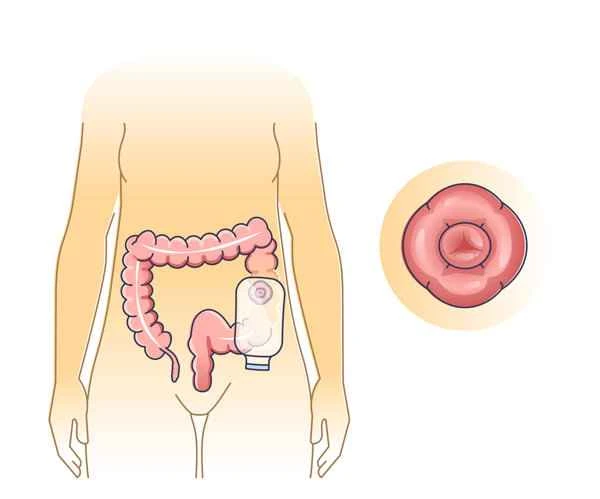
Risk factors for intestinal obstruction include the type of surgery, surgical site, duration of surgery, and postoperative care. The risk of postoperative intestinal obstruction is also closely related to the patient's overall health, such as the presence of chronic diseases, nutritional status, and immune function. In some cases, intestinal obstruction may be temporary and can be relieved through non-surgical treatments such as fasting, gastrointestinal decompression, and fluid replacement. In other cases, intestinal obstruction may require emergency surgical intervention to prevent serious complications such as intestinal perforation and peritonitis. Timely identification and management of postoperative intestinal obstruction are crucial for preventing serious consequences.
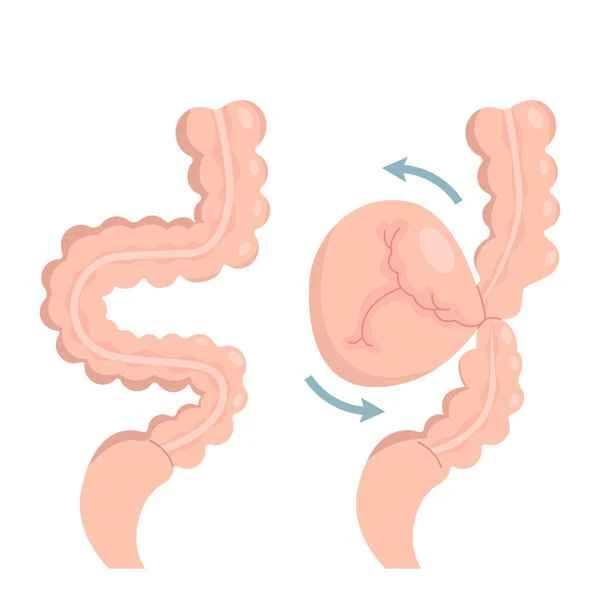
[Management Tip:]
1. Regularly monitor abdominal symptoms, such as abdominal pain, bloating, and vomiting.
2. Maintain good postoperative care and follow your doctor's instructions regarding diet and activities.
3. If symptoms of intestinal obstruction occur, seek medical attention promptly for evaluation and treatment.