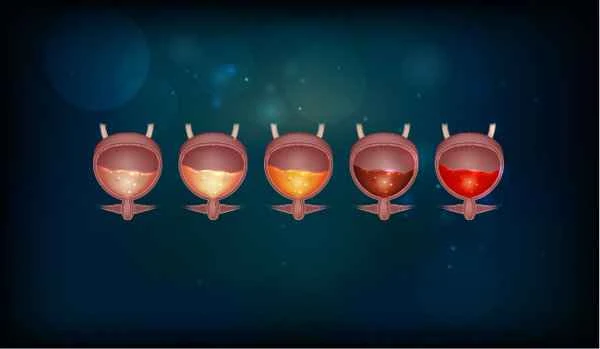
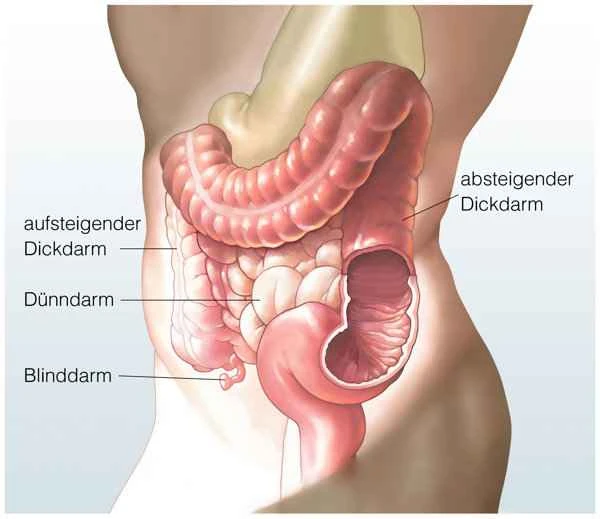
Intestinal obstruction is a condition in which intestinal contents cannot pass through normally. Whether a patient can eat and what they can eat during intestinal obstruction depends on the severity of the condition and the doctor's advice.

In cases of intestinal obstruction, eating requires careful consideration. Patients with intestinal obstruction cannot achieve normal bowel movements, preventing food and fluids from passing smoothly through the intestines, leading to symptoms such as vomiting, abdominal pain, and bloating. During the acute phase of intestinal obstruction, fasting is usually necessary to reduce the burden on the intestines and prevent the condition from worsening. At this stage, patients typically require intravenous fluid therapy to replenish fluids and nutrients and maintain electrolyte balance. As the condition improves, doctors will gradually reintroduce a diet based on the patient's specific situation. This process usually begins with liquid foods, gradually transitioning to semi-liquid foods, and finally returning to a normal diet. This gradual approach helps reduce the burden on the intestines and promotes the recovery of intestinal function.
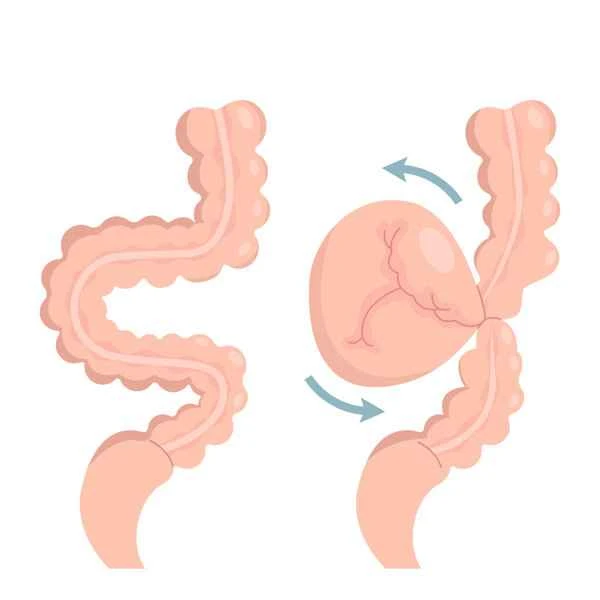
During the treatment of intestinal obstruction, patients may encounter some misconceptions. For example, some patients may believe that as long as they fast, the intestinal obstruction will improve naturally. However, the treatment of intestinal obstruction requires comprehensive consideration of multiple factors, including the cause, severity of the condition, and complications. During treatment, patients need to closely monitor changes in their symptoms and communicate with their doctors promptly to adjust the treatment plan. Patients may experience complications during treatment, such as intestinal perforation and intestinal necrosis. These complications can be life-threatening and therefore require timely detection and management.

[Management Tip:]
1. During the acute phase of intestinal obstruction, it is necessary to fast and replenish body fluids and nutrients through intravenous infusion.
2. After the condition improves, gradually resume a normal diet, starting with liquid foods and gradually transitioning to a normal diet.
3. During treatment, closely monitor changes in your symptoms and communicate with your doctor promptly to adjust the treatment plan.